Intacs for Keratoconus in Los Angeles
Dr. Brian’s Very First Intacs® for Keratoconus Patient 20 years ago
Intacs® Help Improve Your Vision
In 2003, Intacs were approved by the FDA for the treatment of keratoconus. Intacs are tiny, clear, semi-circle inserts that are placed in the peripheral layer of the cornea to help reshape the steep area of the cornea. This procedure is quick, painless, and performed in the comfort of Dr. Brian’s office procedure room.
There is help for you to improve your vision and end the anxiety and suffering. To achieve maximum impact on keratoconus and improvement in your vision, Dr. Brian typically combines Intacs with the Holcomb C3-R® Crosslinking System. Most patients typically have both procedures performed on the same day.
Dr. Brian’s Approach with Intacs
Dr. Brian pioneered Intacs for keratoconus in 1999. Dr. Brian does not use sutures, he invented the technique of dissolvable tissue glue instead of stitches during the procedure. Dr. Brian Boxer-Wachler has the most experience in the world with Intacs and performs more Intacs procedures in a week than most surgeons will perform in a whole year.
Dr. Brian’s technique and his large research study were used by the FDA as part of their approval. The FDA adopted part of his procedure guidelines for the approved Intacs® technique which is the basis for instructional courses used to train other surgeons around the world.
How Do Intacs® Work?
Intacs® reshape the curvature of the cornea from within to flatter part of the bulge. No tissue is removed, so natural optics are enhanced without detracting from the structural integrity of the cornea. As a result, a curved glide creates a channel in the periphery of the cornea by gently separating the tissue layers. One or two tiny plastic Intacs® are placed in the channel much like placing a pencil in between the pages of a book. This causes the cornea to flatten which helps achieve clearer vision.
Dr. Brian invented the L-U® ophthalmic tool which is used to measure corneal irregularly. We have found that Intacs® improve the irregular corneal shape. This typically translates into improved vision with less distortion, glare, streaking of lights and help night vision too.
Benefits of Intacs® for Keratoconus
- 7-minute outpatient procedure.
- Completely memovable and exchangeable.
- Improved quality of vision.
- Sharper vision, less glare, less distortion and less double vision.
- Improved night vision.
- Less invasive than cornea transplants.
- Helps prevent cornea transplants when combined with Holcomb C3-R®.
- Doesn’t preclude one from undergoing a corneal transplant in the future if needed.
Potential Risks of Intacs® for Keratoconus
- Foreign body sensation.
- Glare/halos.
- Infection.
- No improvement.
- Sub-optimal vision.
Not everyone with keratoconus will be a candidate for the Intacs® procedure. Only an experienced eye doctor like Dr. Brian Boxer-Wachler can determine if you are a candidate for Intacs®.
Edith Improves Her Vision With Intacs
Steven Holcomb’s Inspirational Story About His Keratoconus Experience
The Most Experienced Intacs® Expert in the World
Dr. Boxer-Wachler has the most experience in the world performing Intacs® for Keratoconus. Patients fly from all over the world because they want their precious eyesight in the hands of “The Keratoconus Guru” and won’t settle for anything less.
Dr. Brian’s TEDX Talk On Pioneering Holcomb C3-R For Keratoconus
Questions To Ask Your Intacs® Surgeon
If you are considering other surgeons for your Intacs® procedure, you may want to ask about their level of experience with Intacs® and if they send your information to an outside consultant to be told how to perform the procedure. The expertise that is required for planning and performing an Intacs® procedure is highly complex and requires years of experience.
- Will 1 or 2 segments be used?
- What thickness will be used?
- What location will Intacs® be placed?
- Do you perform the Holcomb C3-R® Crosslinking System combined with Intacs®?
Intacs® without Holcomb C3-R® only addresses 50% of the keratoconus problem. Keratoconus needs to be halted and your vision must be improved in the best possible manner.
Your cornea is soft and moldable making it ideal for the placement of Intacs® to reshape the cornea and flatten the cone. Then immediately after placement, Holcomb C3-R® helps to improve the firmness of the cornea. This is the reason it is best to combine both procedures on the same day, rather than coming back later for Intacs®.
Risks of Putting Off Keratoconus Treatment
I have treated thousands of patients just like you. A couple whose teenage son had keratoconus delayed seeking treatment resulting in the loss of most of his vision in both eyes. I had another patient who believed her eye doctor when he told her that hard contact lenses hold back keratoconus. Sadly, that was not the case and she lost vision year after year while her eye doctor kept cashing in by updating her contact lenses. Another patient was told he had keratoconus but his eye doctor simply said, “There isn’t much you can do but wait until it gets bad enough for a cornea transplant.” He lost more vision over the years by waiting. These are a few of the thousands of stories I’ve heard over the years – people whose keratoconus was holding them back from realizing their hopes and dreams.
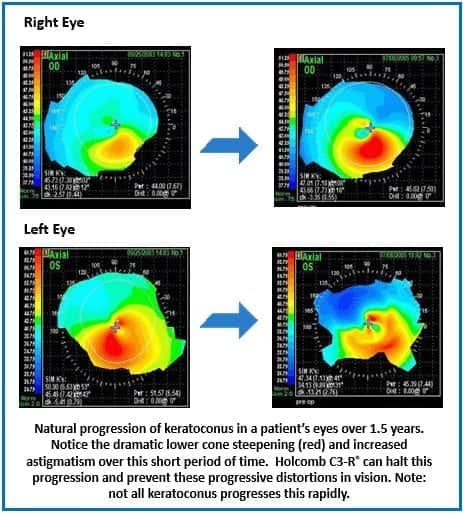
Keratoconus is unpredictable and progressive. Holcomb C3-R® is recommended at a minimum to strengthen your cornea and help prevent future vision loss. If your keratoconus isn’t bad right now, this is the time to do something before it gets worse. Your corneas will continue to bulge out and you will lose more vision. The risk of waiting is that as your corneas continue to bulge out and get worse, the back layer of the cornea can rip open like someone splitting their pants. When this happens to the progressively bulging cornea, the internal eye liquid rushes in and swells up the cornea resulting in 3-6 months of lost vision until this fluid dissipates. Afterward, the cornea will have a lot of new scarring, and vision will be permanently worse compared to before it ripped open. This devastating damage can easily be prevented with the 30-minute, non-invasive, 1-day recovery Holcomb C3-R®.
Out-of-Town Patients
If you live out of town, that’s not a problem. I am are happy to help by providing a complimentary record review prior to you scheduling an appointment.
When you contact us, you will receive your own personal keratoconus counselor to assist you with this process. Your keratoconus counselor will coordinate a review of your records with me. Then your keratoconus counselor will personally contact you to discuss my preliminary recommendations. Then when you are ready, your keratoconus counselor will help you schedule a visit for the exam, treatment, and follow-up exam all within the same easy 3-day visit.
Your keratoconus counselor can also help coordinate your local follow-up doctor. Think of your keratoconus counselor as virtually being with you every step of the way, by your side, from your initial contact with the office through the return home for your follow-up care.
How to Contact Keratoconus Specialist
Here’s how to submit your records for me to review.
- Request a copy of your most recent eye exam from your eye doctor – be sure they include your manifest refraction (prescription) with best corrected vision.
- Request a copy of your most recent color cornea mapping (topography), along with your last 2 or 3 eye exams.
- Write a brief cover letter explaining your current vision and situation.
- Include on the cover letter the title “Keratoconus Record Review” as well as the best phone number and e-mail to contact you.
- Scan and e-mail to: info@boxerwachler.com
Mail to: Boxer Wachler Vision Institute Keratoconus Record Review
465 N. Roxbury Drive, Suite 902 Beverly Hills, CA 90210
Or you can scan your records and email them to info@boxerwachler.com.